In this post, OrthoBuzz spotlights JBJS video and audio content connecting members of the orthopaedic community around the globe. Video JBJS Essential Surgical Techniques (EST)
Category: Need to Know

The rigorous evaluation of manuscripts submitted to JBJS would not be possible without the many Consultant Reviewers from around the world who contribute their knowledge
The OrthoJOE podcast is celebrating its 100th episode. You can access the milestone episode and the full OrthoJOE archive here. Launched in 2021 as a

One year ago, JBJS organized the Sex and Gender Reporting in Musculoskeletal Research Symposium (SGS). The meeting provided an opportunity for focused discussion of: How
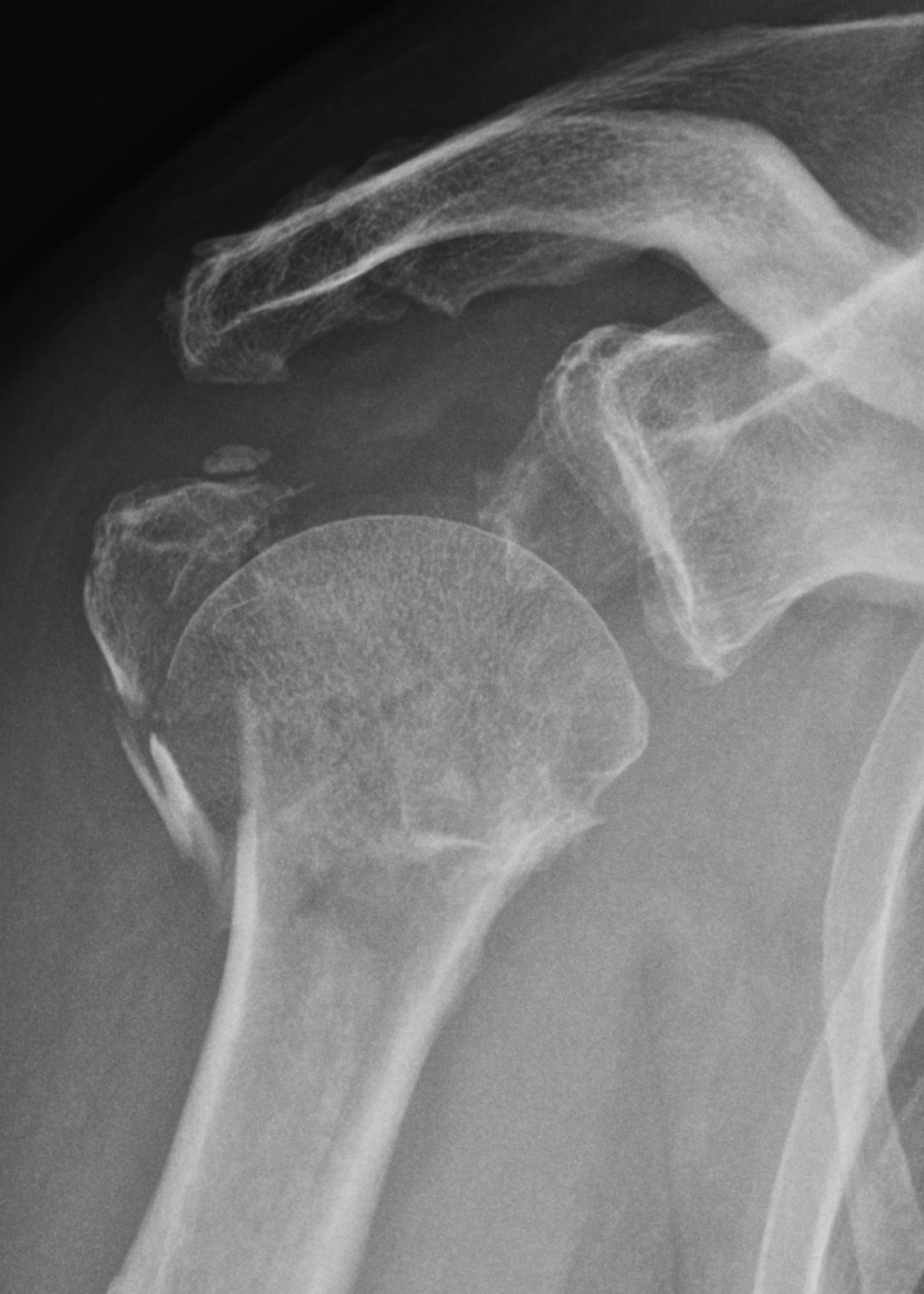
Now in JBJS, Fraser et al. present the 5-year results of the DelPhi (Delta-PHILOS) trial, a multicenter, single-blinded randomized controlled trial. The researchers evaluated reverse

A new special digital collection brings together the most-read JBJS Hip and Knee articles from the past 2 years. Including recent papers on hip and
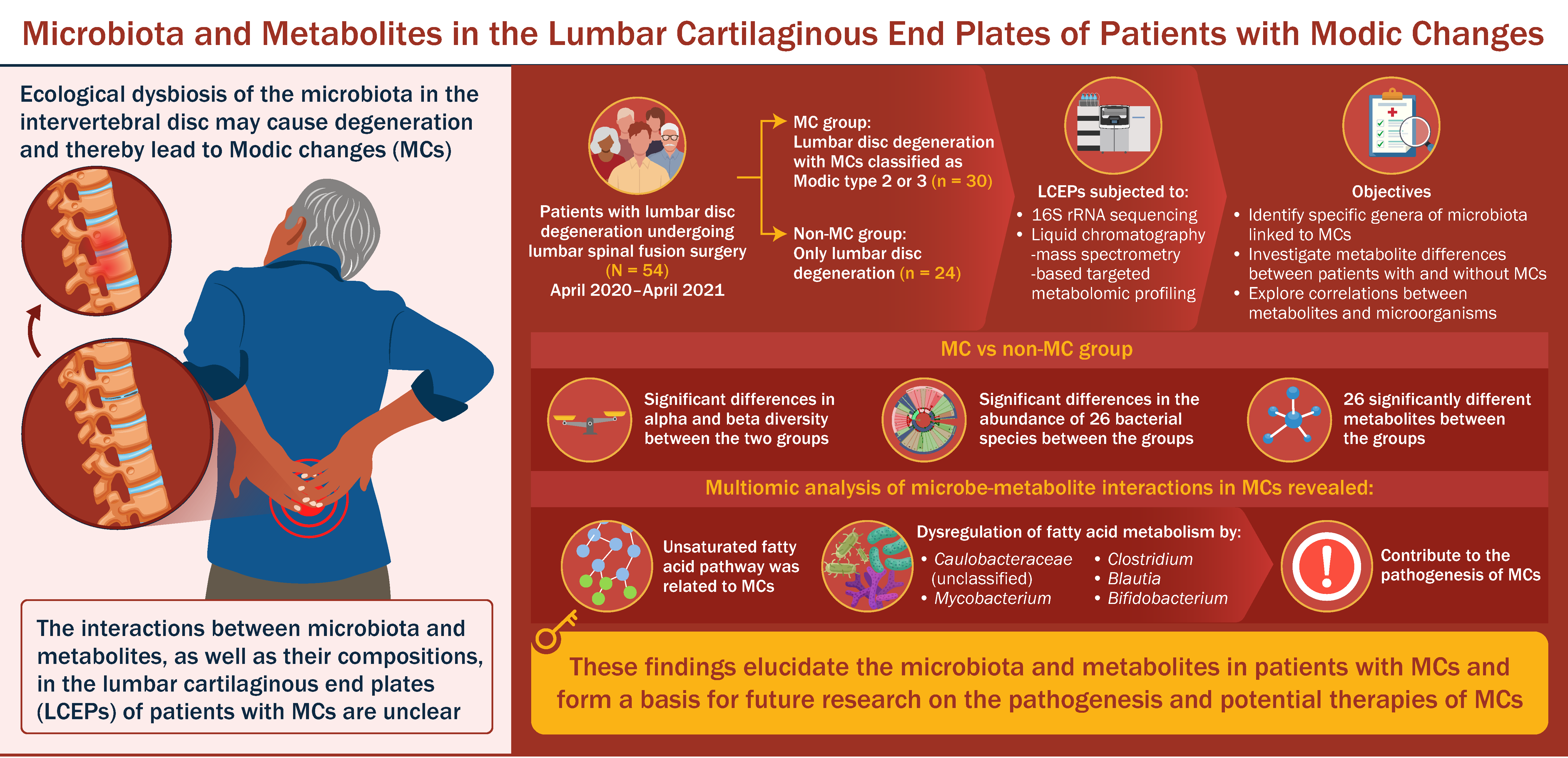
As reported recently on OrthoBuzz, a study by Nian et al. provides novel exploration of microbiota and metabolites in patients with Modic changes—changes in vertebral
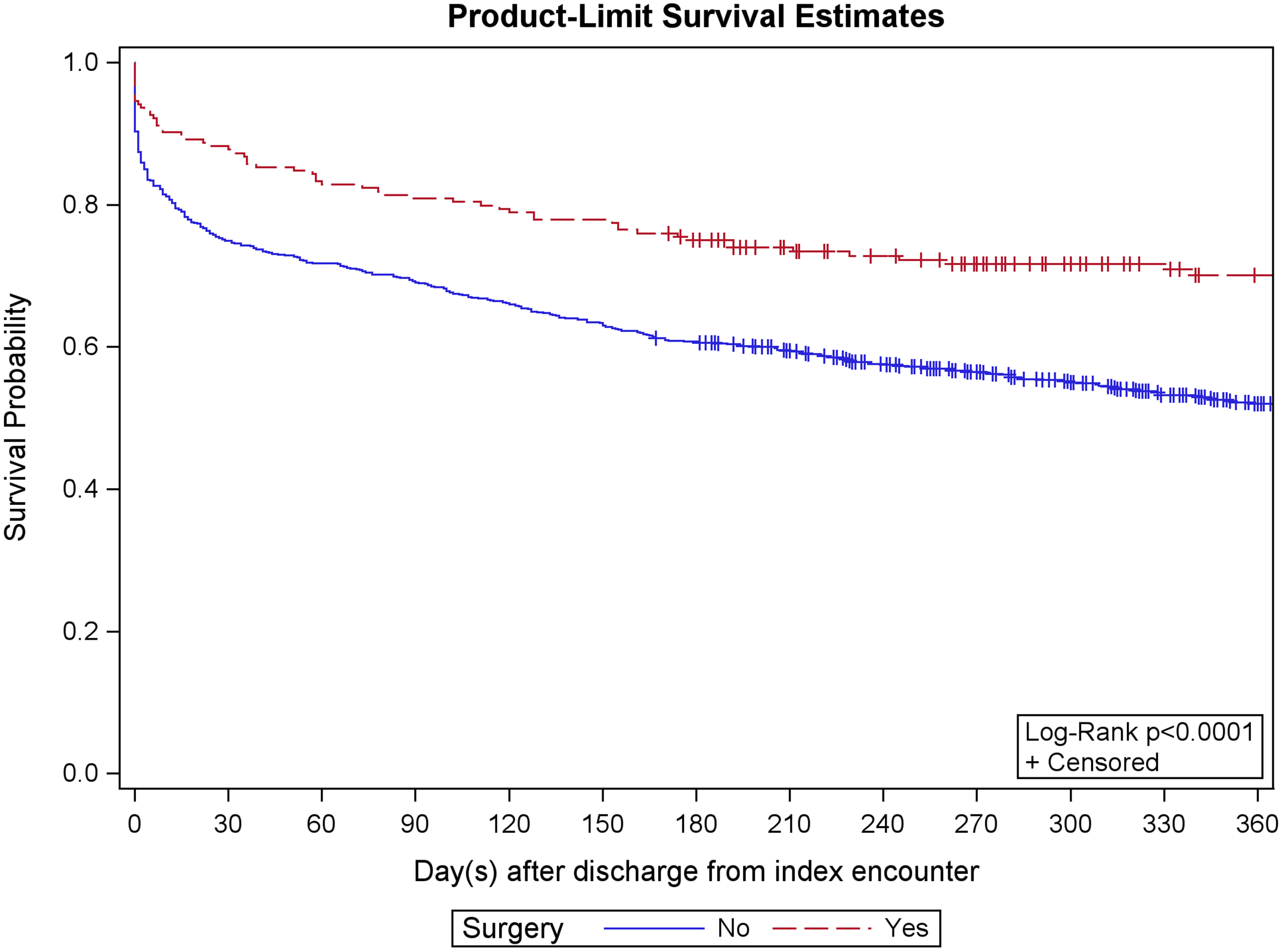
In a new study in JBJS, investigators found that surgical intervention “may confer a survival benefit” in elderly patients with dementia who sustain a type-II

Research is the foundation of countless achievements in science and medicine—and the shared calling of many in the orthopaedic community around the globe. In this

Whether you’re preparing for the ABOS or FRCS exam, JBJS has two outstanding educational programs available to residents and early-career surgeons. Prep Courses for the

