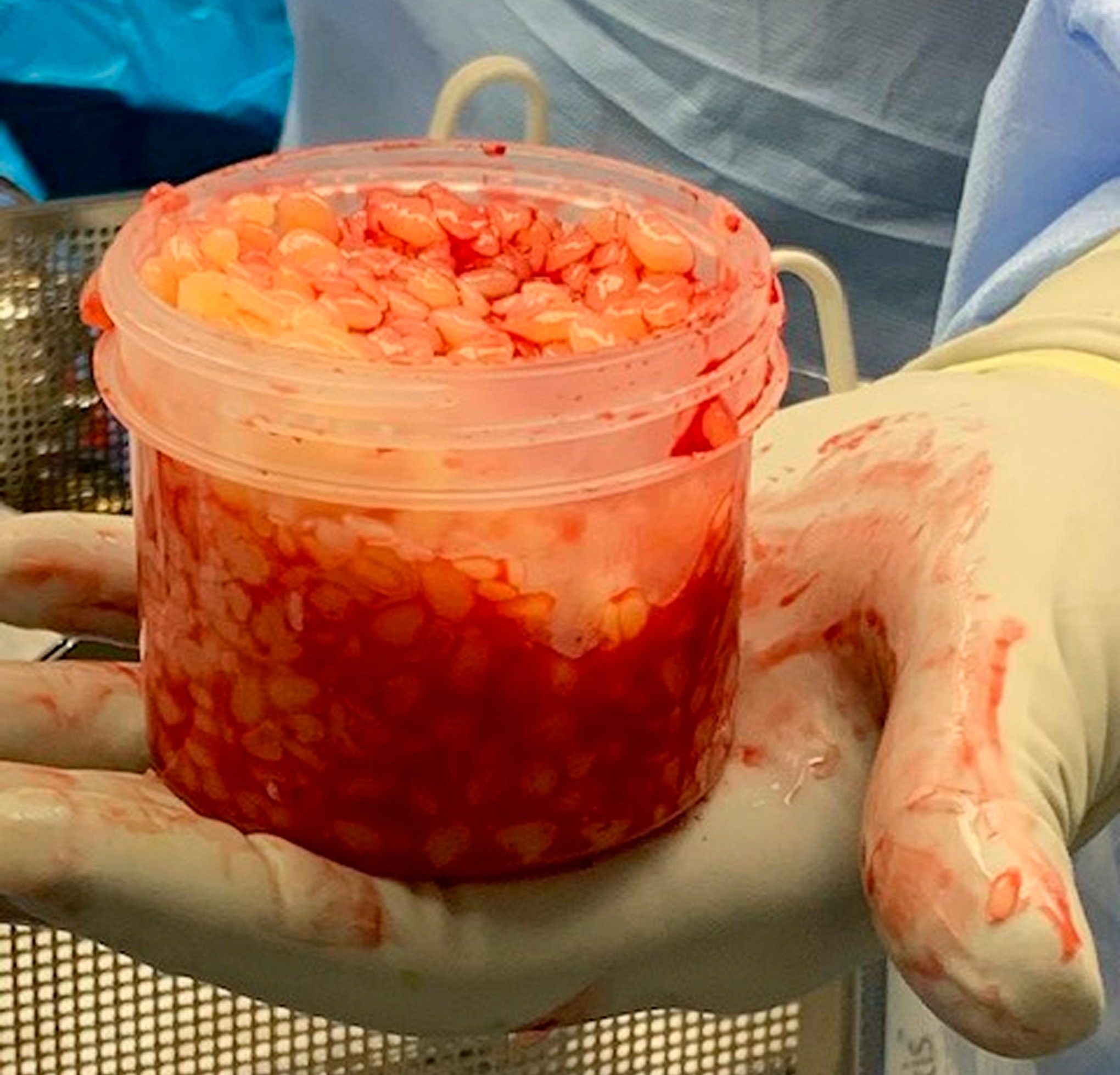
Recent reports in JBJS Case Connector describe 2 orthopaedic cases involving the formation of “rice bodies,” fibrinous loose bodies with a rice-like appearance. As discussed
Category: Shoulder

Topics of interest in the new JBJS Guest Editorial “What’s New in Sports Medicine” include opioid-sparing analgesia, risk of graft failure following meniscal allograft transplantation,
Rotator cuff repair, shoulder arthroplasty, shoulder instability, and the treatment of elbow injuries are among the topics of recent studies reviewed in the new JBJS

Co-author Rachel M. Frank, MD summarizes the 5 most compelling findings from among the studies highlighted in the new “What’s New in Sports Medicine” in JBJS.

This OrthoBuzz guest post comes from Paul E. Matuszewski, MD, in response to a recent article in the New York Times. The ever-increasing importance of
Every month, JBJS publishes a review of the most pertinent and impactful studies from the orthopaedic literature during the previous year in 14 subspecialty areas. Click here for a collection of all such OrthoBuzz Guest Editorial summaries.
Patient surveys are now being widely used by hospital systems to monitor patient satisfaction with the process of inpatient and outpatient musculoskeletal care. While data from the surveys can help guide
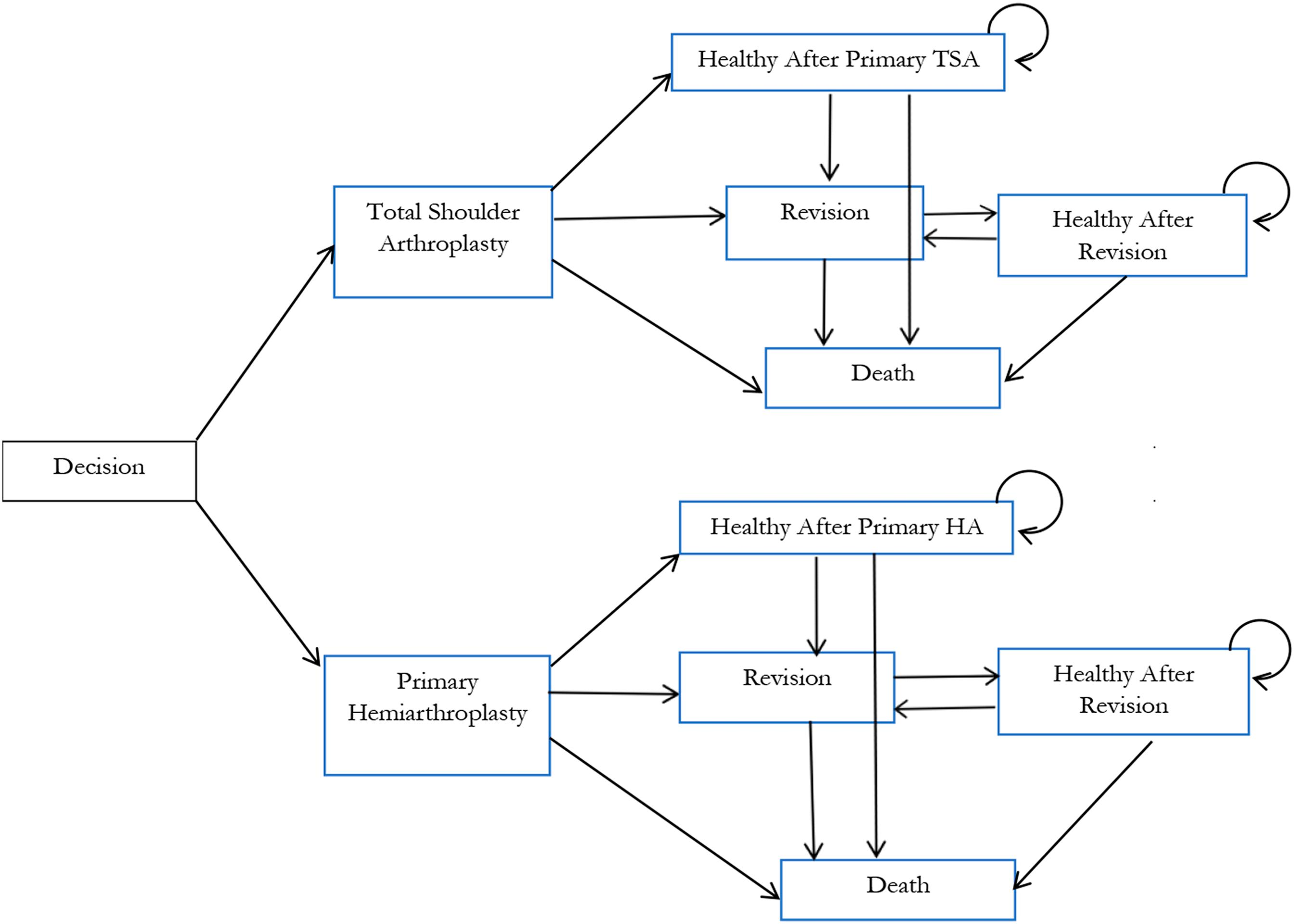
In a new study reported in JBJS, Lapner et al. conducted a cost-utility analysis of total shoulder arthroplasty (TSA) versus hemiarthroplasty from the perspective of Canada’s publicly funded health-care system. They used
Approximately 18% of JBJS scientific studies published in 2020 were Level I or II investigations. The number of high-level studies has continued to grow slowly year over year.
Pain is a remarkable and, at times, poorly understood concept. There has been extensive research showing that patients with the same conditions can experience pain differently and that pain and activity