Dr. Matt Schmitz, JBJS Deputy Editor for Social Media, discusses a new study examining the outcomes of periacetabular osteotomy in patients with borderline hip dysplasia.
The periacetabular osteotomy (PAO) has proven to be an effective strategy for correcting adult hip dysplasia. However, there are still unanswered questions with regard to its use for “borderline” acetabular dysplasia, a term used to describe a lateral center-edge angle (LCEA) of 18° to 25°.
In the current issue of JBJS, Nepple et al. examine the outcomes of PAO in the setting of borderline dysplasia in a large cohort of patients.
Outcomes of Periacetabular Osteotomy for Borderline Acetabular Dysplasia
The authors reviewed a database of prospectively collected data to identify patients who underwent PAO for symptomatic instability with borderline acetabular dysplasia. The procedures were performed by a single experienced surgeon.
Included in the analysis were 186 hips with at least 1 year of clinical follow-up (80.2% of an original cohort of 232 hips identified for inclusion). The mean follow-up was 3.3 years, and the mean patient age was 25.2 years (range, 14 to 45 years); 88.2% of the patients were female.
All of the hips had little to no signs of arthritis (140 hips: Tönnis grade 0 and 46 hips: Tönnis grade 1). Thirty hips (16.1%) had previously undergone hip arthroscopy, at an average of 2.6 years prior (range, 0.5 to 8.3 years). At the time of PAO, additional surgical procedures were performed concurrently in 165 hips (88.7%), with 130 hips undergoing arthroscopy for the treatment of intra-articular pathology and 120 hips undergoing open femoroplasty.
The authors reviewed complications and radiographic and clinical outcomes. They defined clinical failure as a reoperation for persistent symptoms or failure to reach the minimal clinically important difference (MCID) or patient acceptable symptom state (PASS) for the modified Harris hip score (mHHS).
Study Findings
The authors found obvious improvements in radiographic measurements of dysplasia as well as significant improvements from baseline in patient-reported outcomes, including the mHHS and Hip disability and Osteoarthritis Outcomes Score (HOOS):
- mHHS: 58 to 86
- HOOS-Pain: 52 to 83
- HOOS-Sport: 39 to 76
Although there were 5 major complications (2.7%) that required additional surgery, all 5 patients reached the MCID or PASS for the mHHS after reoperation.
Interestingly, the investigators found that the clinical failure rate was higher for hips that had previously undergone arthroscopy vs. those that had not, despite their being no difference in the rate of major complications between the 2 groups. Of the 156 hips with no prior arthroscopy, 2 hips (1.3%) underwent reoperation for persistent symptoms and 6 hips (3.8%) failed to achieve either the mHHS MCID or PASS, for an overall clinical failure rate of 5.1%. In the 30 hips that had undergone a previous arthroscopy, 1 hip (3.3%) underwent reoperation for persistent symptoms and 6 hips (20%) failed to achieve either the mHHS MCID or PASS, for an overall clinical failure rate of 23.3%.
These noted differences in failure rates were seen despite their being no significant differences between the groups in follow-up duration, patient age and body mass index, or dysplasia severity. The prior arthroscopy group did have lower preoperative patient-reported outcomes for the UCLA activity score, HOOS-Sport, HOOS-Symptom, and HOOS-Quality of Life.
Overall, this research shows the utility of PAO (with associated surgeries such as arthroscopy and femoroplasty) in hips that are classified as “borderline” dysplastic. Although there has been a push to consider arthroscopic treatment alone for hips that fall in the borderline dysplastic category, the findings lend question to the likelihood of success with that tactic alone.
The study helps elucidate that further research is clearly warranted in this realm of the evolving specialty of hip preservation in orthopaedics.
Access the full report at JBJS.org.
Additional perspective is provided by Steven A. Olson, MD in the JBJS commentary article: “Managing Borderline Dysplasia: It Can Take More Than Just a Periacetabular Osteotomy.”
JBJS Deputy Editor for Social Media

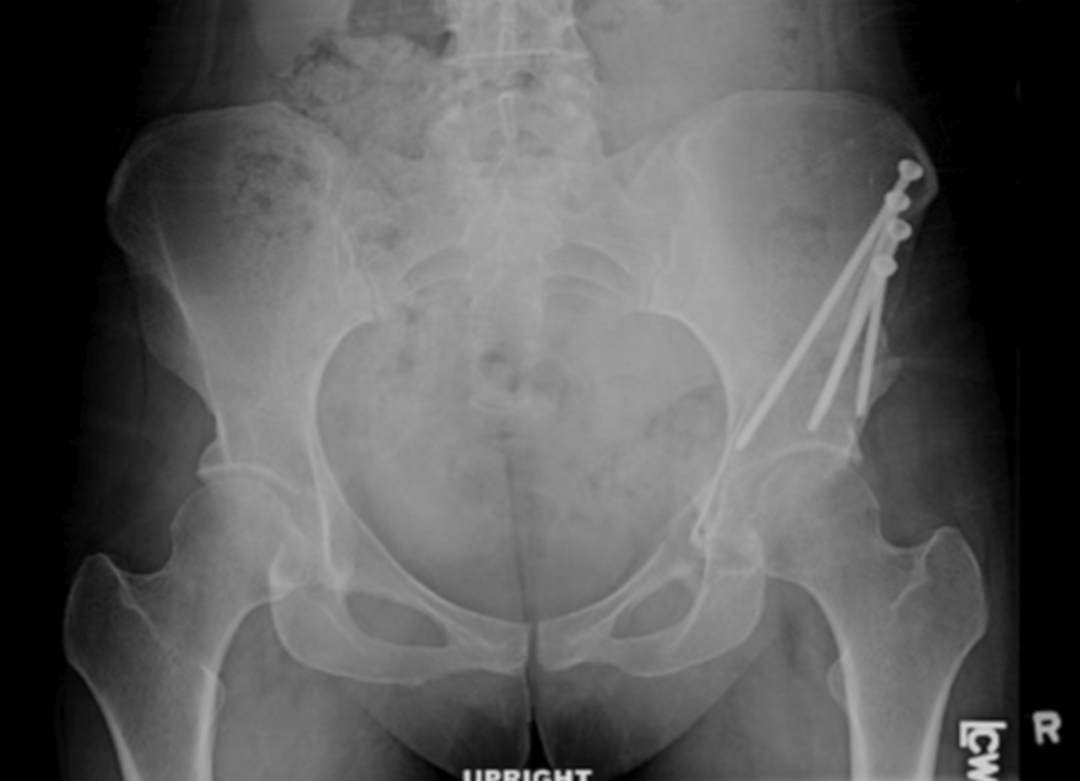



This article is the last one of a long list which demonstrates that the exact and precise coverage (axial, vertical projection of the acetabulum onto the femoral head (norm: 70%)) is essential for aiming at a good result through planning and 3D preop simulation