Recent reports in JBJS Case Connector describe 2 orthopaedic cases involving the formation of “rice bodies,” fibrinous loose bodies with a rice-like appearance. As discussed by the authors, rice body reactions have been observed within joints, bursae, and tendon sheaths. While the precise etiology is not fully understood, rice bodies have been described as a response to chronic inflammation associated with autoimmune conditions and mycobacterial or other infections. An association with orthopaedic implants has been reported in a limited number of cases.
Ramirez et al. describe a case of periprosthetic rice bodies 3 years after metal-on-metal hip resurfacing arthroplasty (HRA) in a 65-year-old man with osteoarthritis. To the investigators’ knowledge, this is the first documented case of rice body formation in the setting of metal-on-metal HRA and the first associated with an inflammatory adverse local tissue reaction:
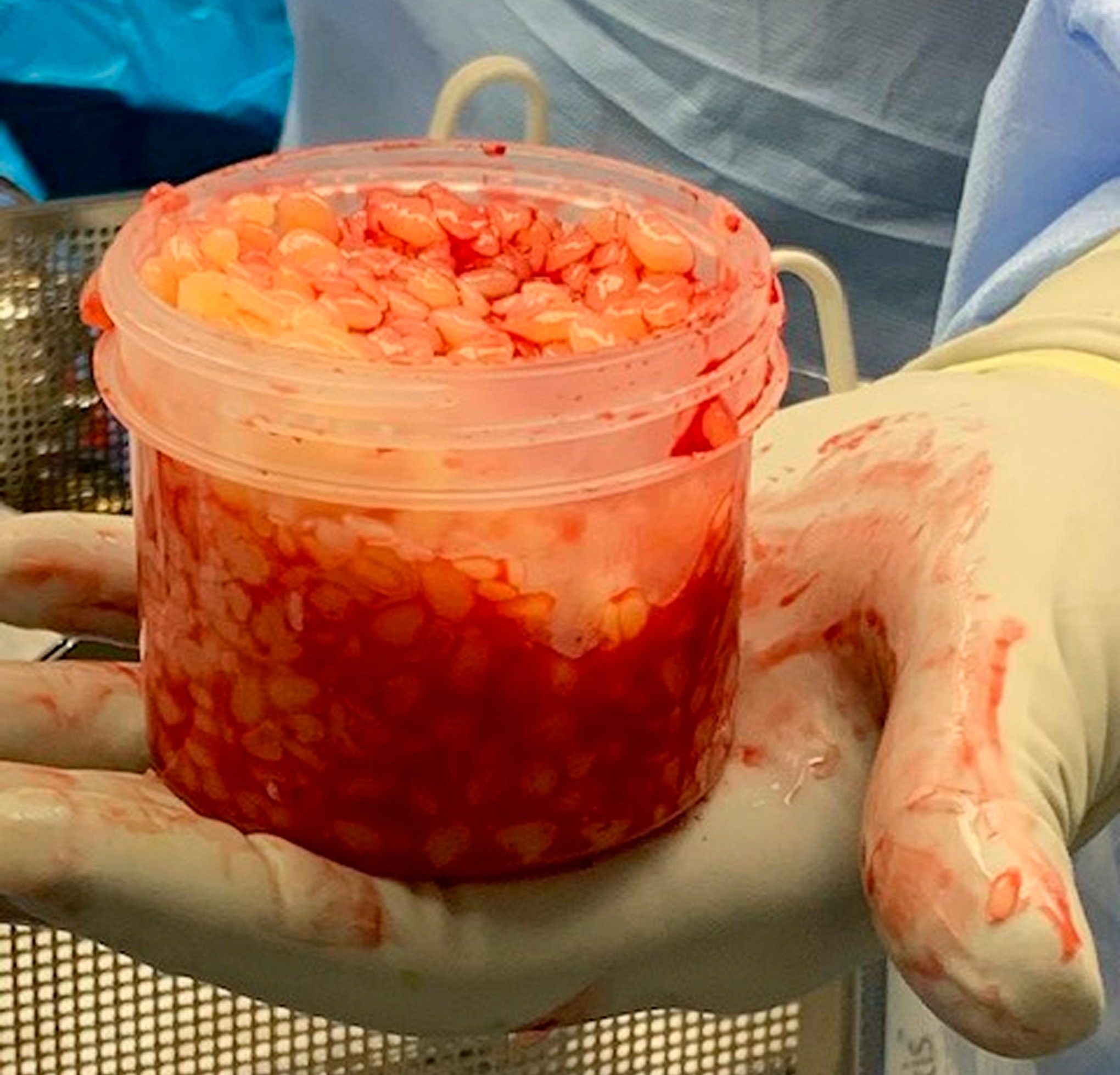
Two years following metal-on-metal HRA, the patient had intermittent groin and medial thigh pain and developed a soft-tissue mass of the inferior gluteal area. An adverse local tissue reaction was suspected on the basis of clinical and imaging findings. Intraoperatively, nearly 1 liter of intra-articular rice bodies was removed. No evidence of osteolysis, necrotic tissue, or infection was found, and the patient underwent conversion to total hip arthroplasty with elimination of the metal-on-metal articulation. Histology demonstrated features of an adaptive immune response. At 6 weeks of follow-up, the patient had full range of motion, and metal ion levels had decreased. At 16 months, he had resumed all activities. Read the case details in the report by Ramirez et al.
The authors note just 8 reported cases of rice body formation in the setting of orthopaedic devices, concluding that, despite their rarity, “it is important to consider this diagnosis in the differential of a slow growing mass adjacent to orthopaedic instrumentation.”
In a separate JBJS Case Connector report, Root et al. present a case of subacromial-subdeltoid bursitis with rice bodies after rotator cuff repair with a collagen scaffold implant:
A 44-year-old man presented to the clinic with shoulder pain. Three years prior, he had been diagnosed with a partial-thickness rotator cuff tear, treated nonoperatively. Because the current pain was interfering with his occupation as a tennis professional and his daily activities, he elected treatment with arthroscopic surgery. Given the specifics of his case, a bovine-derived, bioinductive collagen scaffold implant (REGENETEN; Smith & Nephew) was selected for treatment; a medium-sized patch with 8 polylactic acid tendon anchors and 3 polyether ether ketone bone anchors were used. The patient’s medical history did not include common risk factors for rice bodies.
The patient reported low levels of pain at 10 weeks. Reduced range of motion was noted and thought to be because of reactive synovitis/early adhesive capsulitis, which was addressed by intraarticular glenohumeral corticosteroid injection. While strength improved, range of motion did not advance. At 1 year, the patient had dull and aching pain and reported that the shoulder felt swollen. The authors write, “x-rays revealed loss of the sclerotic border of the undersurface of the acromion, and the MRI revealed significant swelling with debris in the subacromial bursa, containing small bodies of intermediate density. In addition, the MRI showed cystic-like structures eroding both through the deltoid fascia and into the inferior acromion, resulting in local soft-tissue and osseous destruction.”
After removal of the rice bodies and a portion of the implant that had not been incorporated, the patient recovered well, with a full return to activities.
The authors note the rare pathology and limited reports on the occurrence and treatment of isolated subacromial-subdeltoid bursitis with rice bodies after placement of an orthopaedic implant. They conclude that, “This case demonstrates that pain, swelling, or loss of ROM after the use of a rotator cuff patch, implant, or augment with bioresorbable soft tissue staples may warrant an early postoperative MRI to evaluate for this complication and, if diagnosed, may benefit from early surgical intervention.” Read the case details in the report by Root et al.
Other News from JBJS Case Connector on OrthoBuzz
Cellular Bone Matrix Leading to Disseminated Tuberculosis After Spinal Fusion: A Report of 2 Cases
JBJS Case Connector: Call for Reviewers
Disclosure: JBJS Case Connector Co-Editor Thomas Bauer, MD, PhD is a co-author of the article by Ramirez et al. He did not participate in the writing or review of this post.



very nice article very informative