In a new study in JBJS, Asma et al. point out the need for additional evidence-based guidance on radiographic hip surveillance following skeletal maturity in patients with cerebral palsy (CP). Data from the investigation may add to existing guidelines to help identify patients at risk of progression of hip displacement.
The researchers aimed to determine the prevalence of—and risk factors associated with—progressive hip displacement after triradiate cartilage (TRC) closure in children with nonambulatory CP.
- This retrospective cohort study included 163 patients with hypertonic motor type, nonambulatory CP (Gross Motor Function Classification System IV to V). Patients had a mean follow-up of 4.8 years after TRC closure at a mean patient age of 14 years.
- The hip migration percentage (MP) was the primary outcome variable. An unsuccessful hip outcome was defined as an MP of ≥40% and/or the need for a reconstructive surgical procedure after TRC closure.
- Secondary outcome variables included patient age at the time of TRC closure, prior preventive or reconstructive surgery, prior intrathecal baclofen pump, history of scoliosis or epilepsy, prior gastrostomy tube, previous tracheostomy, and gender.
Highlights of Findings
An unsuccessful hip outcome was found for 22.1% of the included patients, at a mean of 37 months after TRC closure.
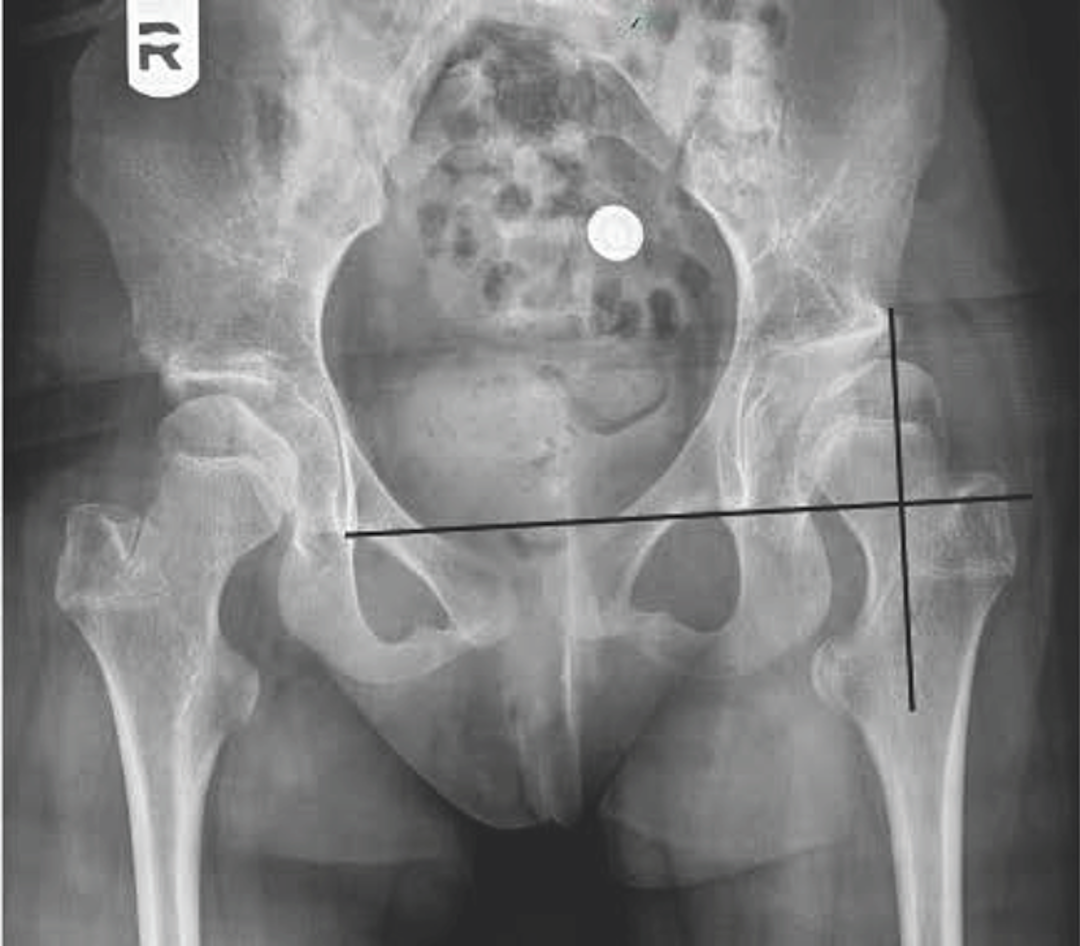
On multivariate analysis, factors associated with an unsuccessful hip outcome were a higher first MP at TRC closure (with each 1% increase in the MP increasing the risk of an unsuccessful hip outcome by 4%) and increased pelvic obliquity at TRC closure (with each 1° increase in pelvic obliquity increasing the risk by 6%).
Survivorship analysis showed that progression to an unsuccessful hip outcome was longer for female patients (mean survival time, 9.2 years) compared with male patients (6.2 years), and was longer for patients who had prior reconstructive surgery compared with no surgery.
A first MP of ≥35% at TRC closure was associated with an unsuccessful hip outcome on ROC analysis.
Conclusions
The authors concluded, “The risk factors for the progression of hip displacement after TRC closure in patients with CP included a higher MP and increased pelvic obliquity; there was decreased survivorship for male patients and patients with no prior reconstructive surgery. Patients with these risk factors and/or an MP of ≥35% at TRC closure should have continued radiographic surveillance to detect late hip displacement.”