A video summary is available with the new Level-I study by Pongcharoen et al. in JBJS, “Comparison of Functional Recovery Between Unicompartmental and Total Knee Arthroplasty: A Randomized Controlled Trial.”
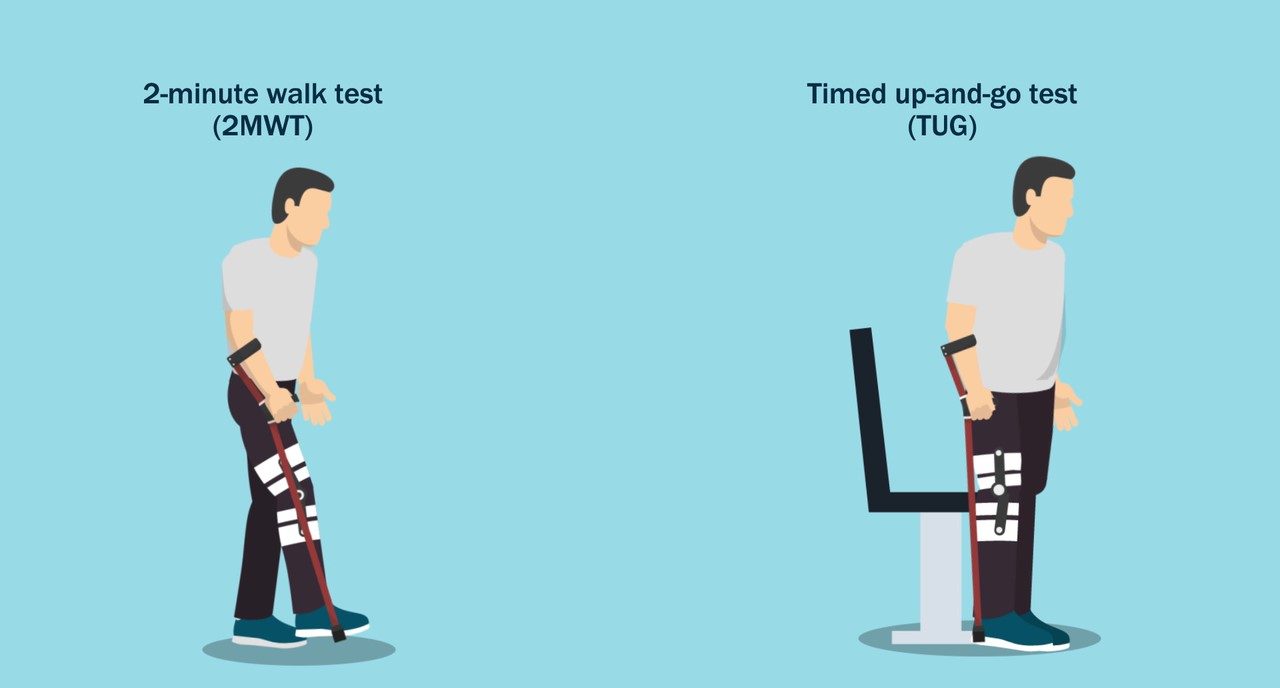
The investigators compared the results of the 2-minute walk test (2MWT) and the Timed Up-and-Go Test (TUG) in patients undergoing unicompartmental knee arthroplasty vs. total knee arthroplasty (UKA vs. TKA) for isolated medial knee arthritis. Patient-reported outcome measures were also assessed.
Watch the video summary:
As concluded by the authors: “The 2MWT indicated that UKA for isolated medial knee OA enabled faster recovery than TKA did at 6 weeks to 6 months, and earlier recovery was also seen with the TUG at 6 weeks to 3 months. The 2MWT and TUG results after UKA and TKA were similar to one another at 1 and 2 years.”
Read the full study by Pongcharoen et al. at JBJS.org.
JBJS Video
Interested in other JBJS video content? Explore the new JBJS Video at JBJS.org, featuring Ortho Procedures, Video Abstracts, Author Insights, and more—all in one place at JBJS.org.



The study looks at any differences between a mobile bearing UKA and a Posterior-stabilised (PS) TKA, the latter generally accepted as resulting in more bone work and excision than Cruciate retaining (CR) TKA alternatives. It is uncertain if the implant fixation were all by cement, although the illustrations supplied in the study suggests at least some were. It is also not stated in the surgical technique if the PS TKA all had patella resurfaced, despite the conventional recommendation that PS TKA systems should routinely have patella resurfacing, a practice that the authors’ own compatriots have recommended (ref 1).
Hence, we are potentially looking at a large contrast in surgery between UKA and TKA techniques particularly with respect to soft tissue and bone work.
Despite this there is in effect no difference in function within 12 months of surgery, any gain or benefit with UKA 6 months post-operatively disappearing by then.
However there is a matter not directly addressed by the study; it is generally accepted that UKA have a higher revision rate compared to TKA (ref 2-4), although the Thai experience may be different (and better) from the other centres, for both fixed and mobile bearing types (ref 5-6). Of note the average age having knee arthroplasty in this study is mid-sixties, which in other populations will have long enough life-expectancy to oversee a revision of a significant proportion of UKA. Thus, readers from non-Thai centres need to carefully consider the applicability of this study to the population they serve.
As additional comment of interest: the video supplied here seemed to suggest patient post knee replacement would be wearing knee brace for weeks-months post operatively by the time they present for assessment for the tests so described. I haven’t used knee brace routinely for years for any of my knee arthroplasty patients, and I doubt this practice occurs in many Thai centres either, although I cannot be certain if this does occur at Thammasat University Hospital or not.
References:
1. https://pubmed.ncbi.nlm.nih.gov/31126775/
2. DOI: 10.2106/JBJS.18.01468
3. https://doi.org/10.1186/s10195-020-00551-x
4. http://dx.doi.org/10.1016/j.knee.2016.11.006
5.http://www.jmatonline.com/index.php/jmat/article/view/9545#
6. https://doi.org/10.21203/rs.3.rs-583930/v1