In this post, Editor-in-Chief Dr. Marc Swiontkowski discusses a new study in JBJS that assesses the impact of teriparatide use in patients with osteoporosis undergoing spinal fusion.
Surgery for adult spinal deformity has been shown to be effective in terms of improving spinal balance and health-related quality of life. Spinal deformity associated with aging is more common in females than males, with diminished bone density related to hormonal changes after menopause. Osteoporosis is, of course, also a disease experienced by males, although the diagnosis is often not considered or is underdiagnosed in male patients.
Since the advent of anabolic agents for osteoporosis, spine surgeons who treat deformity have been working with endocrinologists to prescribe these medications in an effort to improve the strength of the implant-bone interface to limit the failure of correction. The evidence of the effectiveness of this strategy has generally been lacking to date.
In the February 7, 2024 issue of JBJS, Mohanty and colleagues present new data on the impact of teriparatide in osteoporotic patients treated surgically for adult spinal deformity. Their study, performed at Columbia University Irving Medical Center in New York, is available at JBJS.org:
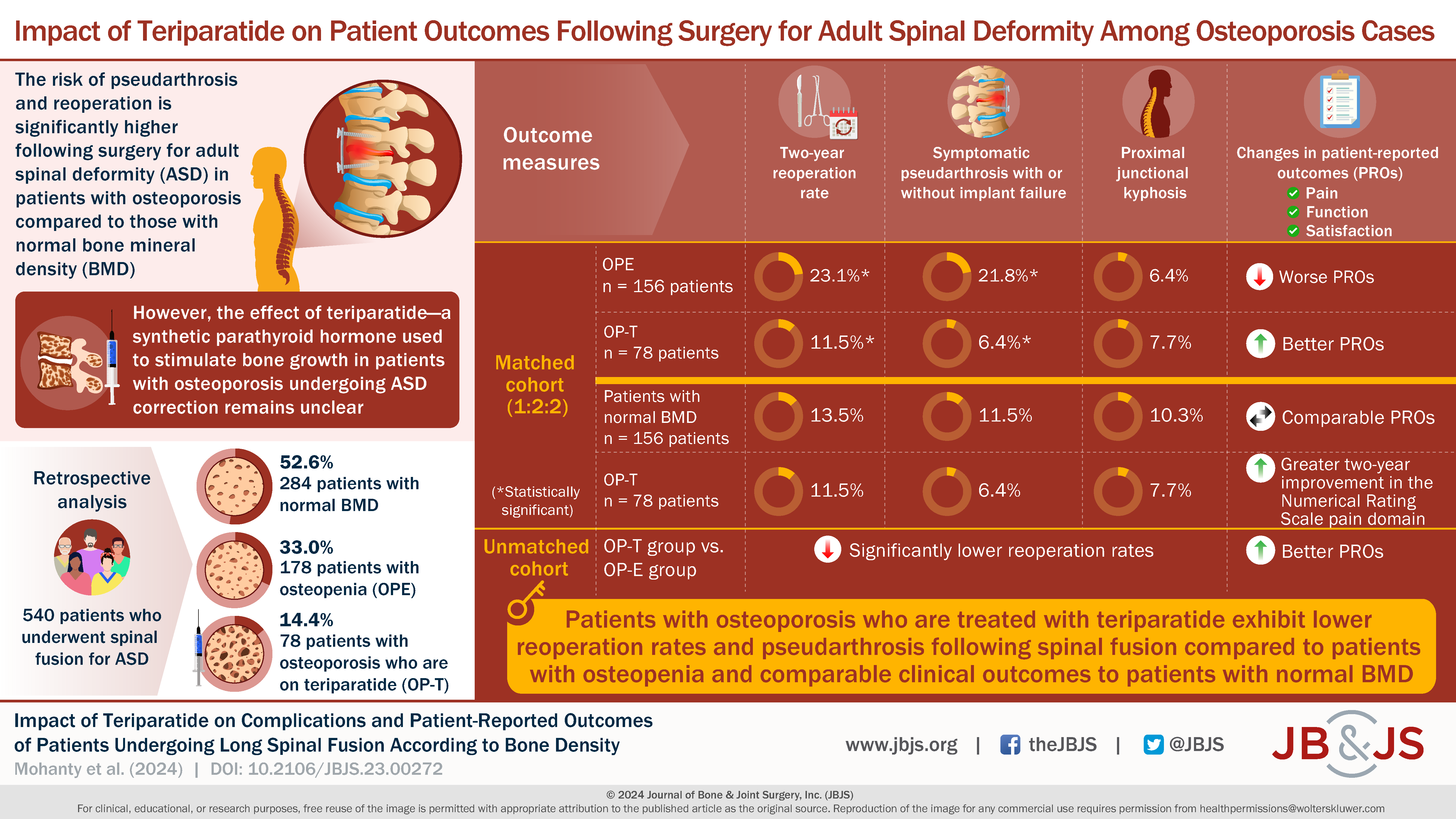
In this retrospective, single-surgeon study, patients underwent posterior spinal fusion involving >7 instrumented levels. Osteoporotic patients receiving teriparatide were compared with patients with osteopenia and patients with normal bone mineral density (BMD). Propensity-score matching was used (1:2:2 ratio). The 2-year reoperation rate was the primary outcome. Pseudarthrosis with or without implant failure, proximal junctional kyphosis, and changes in patient-reported outcomes were secondary outcomes. Bone density was assessed using standard DXA methodology or QCT. A total of 540 patients were included (72.8% female, mean age of 61.9 years). There were 78 patients in the OP-T group, 178 in the OPE group, and 284 in the group with normal BMD.
Study Findings
In the unmatched cohort, the authors found that the group receiving teriparatide had significantly lower rates of 2-year reoperation (odds ratio, 0.45; p = 0.0181) and pseudoarthrosis (odds ratio, 0.25; p = 0.0054) compared with the group with osteopenia. In the matched analysis, the group receiving teriparatide again had significantly lower 2-year rates of reoperation (11.5% vs. 23.1%; odds ratio, 0.45; p = 0.0188) and pseudarthrosis (6.41% vs. 21.8%; odds ratio, 0.25; p = 0.0048) compared with the group with osteopenia.
When compared with the matched group with normal BMD, the osteoporotic group receiving teriparatide had similar rates of reoperation, pseudarthrosis, and proximal junctional kyphosis. The authors also found that patient-reported outcomes did not differ significantly between these 2 groups.
Access the study details: Impact of Teriparatide on Complications and Patient-Reported Outcomes of Patients Undergoing Long Spinal Fusion According to Bone Density
Among limitations, the investigation is impacted by all the issues of a retrospective design, including selection bias. Additionally, it is not clear whether or not the individuals assessing the radiographs were blinded to treatment-group clinical data, a potential source of detection bias. Even so, this carefully analyzed study demonstrates that, in the hands of an expert spinal deformity surgeon, use of an anabolic agent in patients with osteoporosis may create a biologic environment that vastly improves the chances of maintenance of correction obtained at surgery with attendant good clinical and functional outcomes.
Additional perspective is provided by Daniel G. Kang, MD in a related commentary: Does Teriparatide Improve Outcomes in Osteoporotic Patients Undergoing Adult Spinal Deformity Surgery?
JBJS Editor-in-Chief