Recent findings related to bone loss and bone healing, among other important topics, are presented in the new JBJS Guest Editorial What’s New in Musculoskeletal
Category: Pediatrics
In this post, Dr. Matt Schmitz, JBJS Deputy Editor for Social Media, discusses a new study examining the impact of social determinants of health on
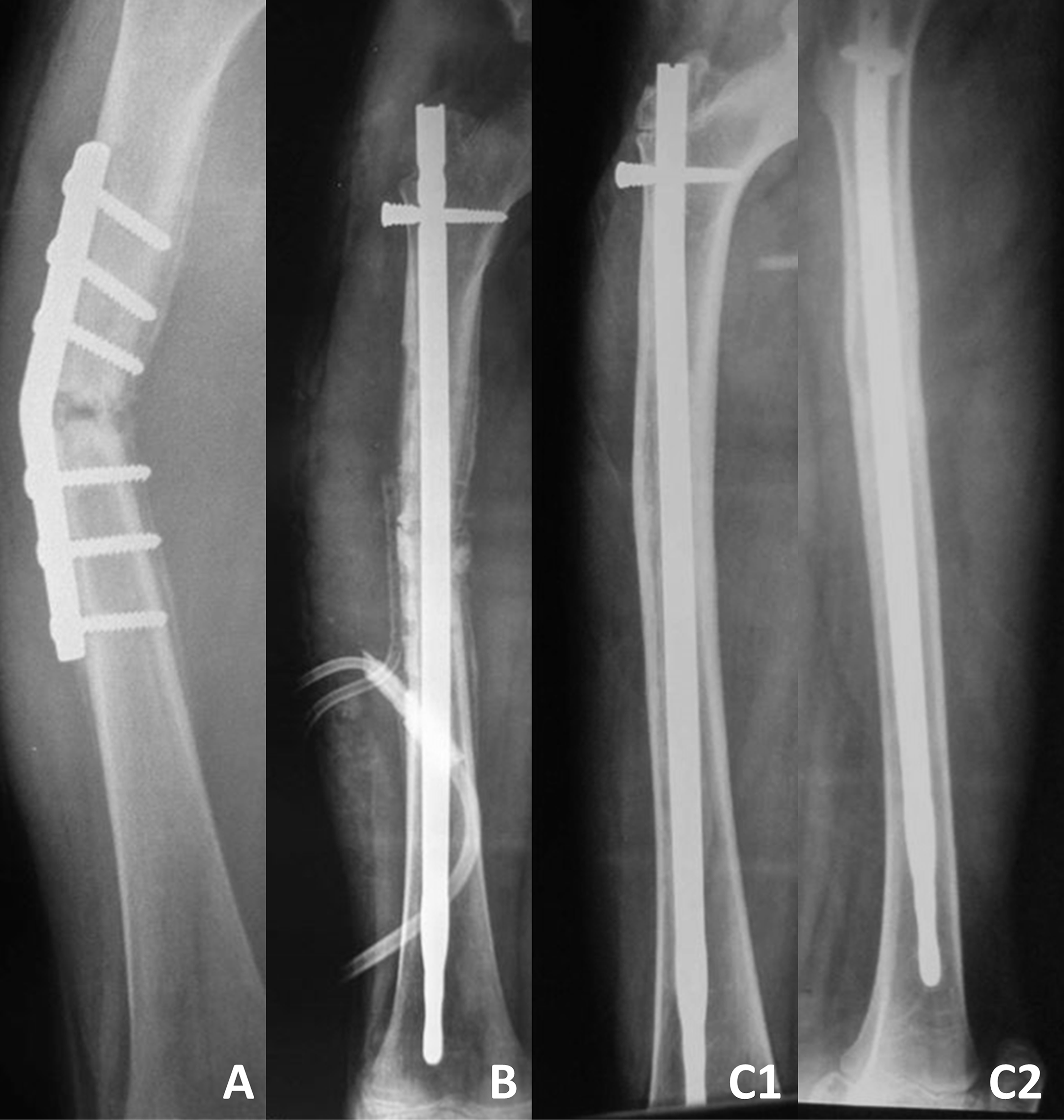
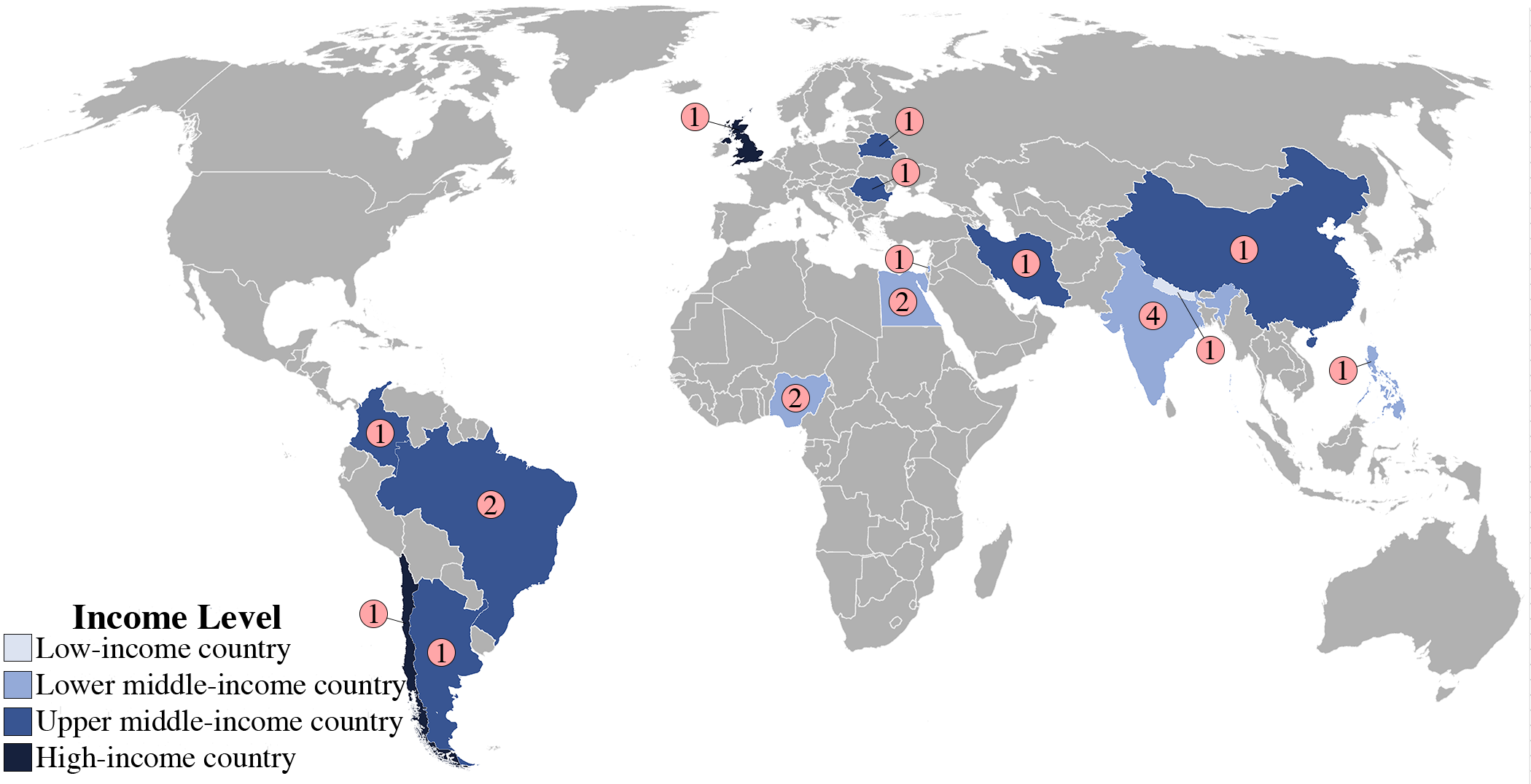
A new study in JBJS evaluates intramedullary fixation for femoral nonunion in pediatric patients in low- and middle-income countries. Dr. Matt Schmitz, JBJS Deputy Editor
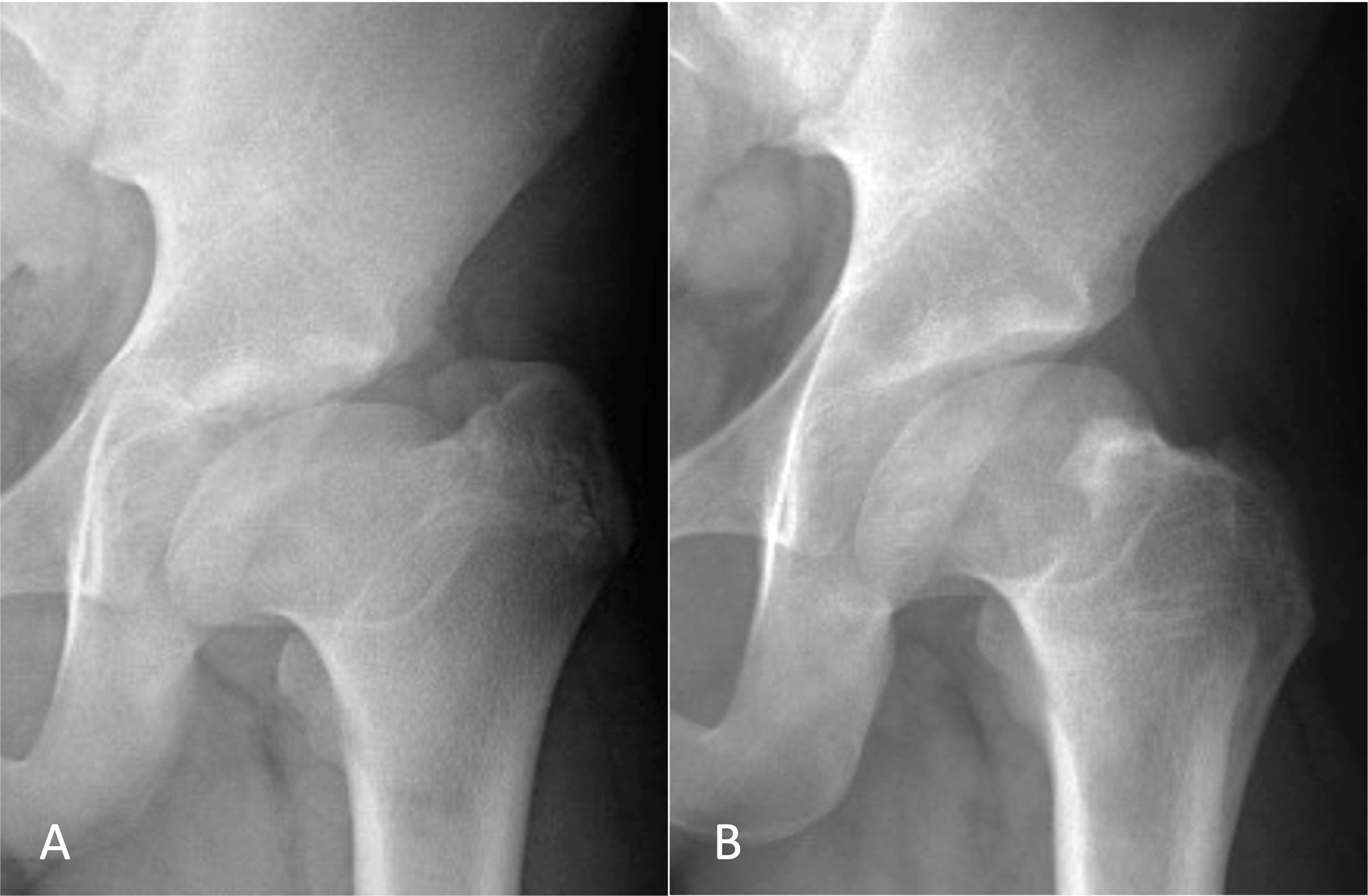
In a new study in JBJS, Novais et al. note the challenge of treating patients with symptomatic hips after healed Legg-Calvé-Perthes disease (LCPD) given the
Collaborative efforts to provide international educational opportunities have been part of the orthopaedic landscape for many years. Some of these experiences involve orthopaedic society-funded traveling
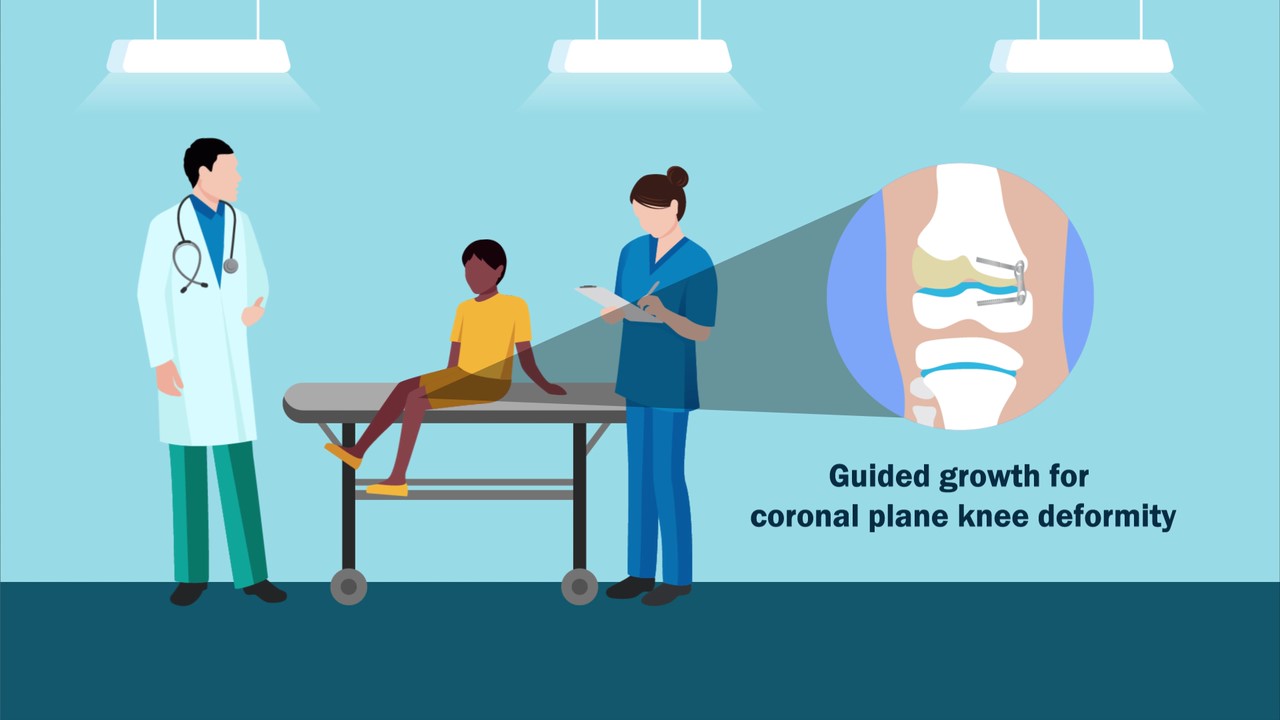
A video abstract is available with the new study by McGinley et al. in JBJS: Faster Rate of Correction with Distal Femoral Transphyseal Screws Versus
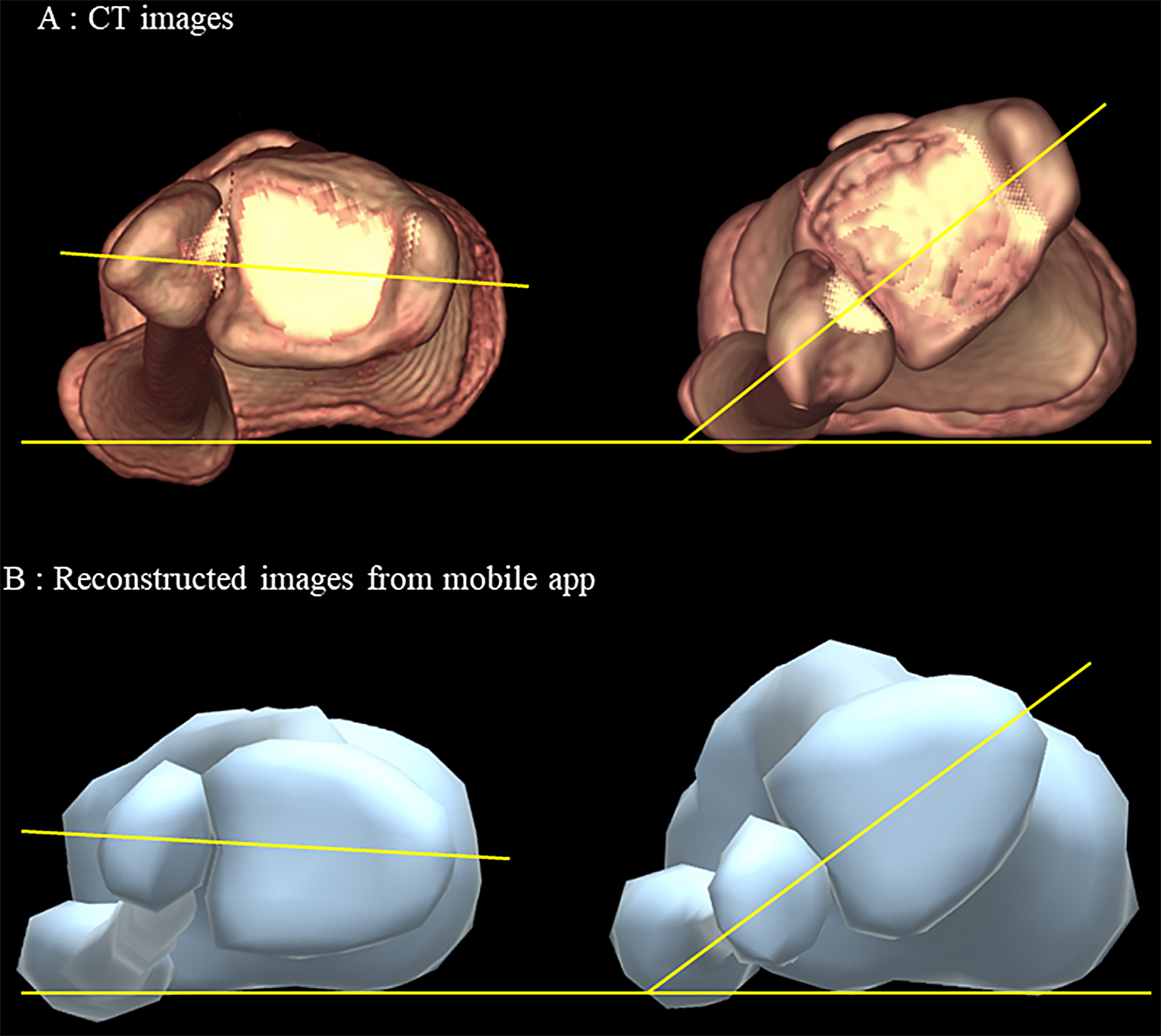
Topics of interest, including a new 3D reconstruction tool for the lower leg, infection rates of pin sites treated with primary closure versus secondary wound
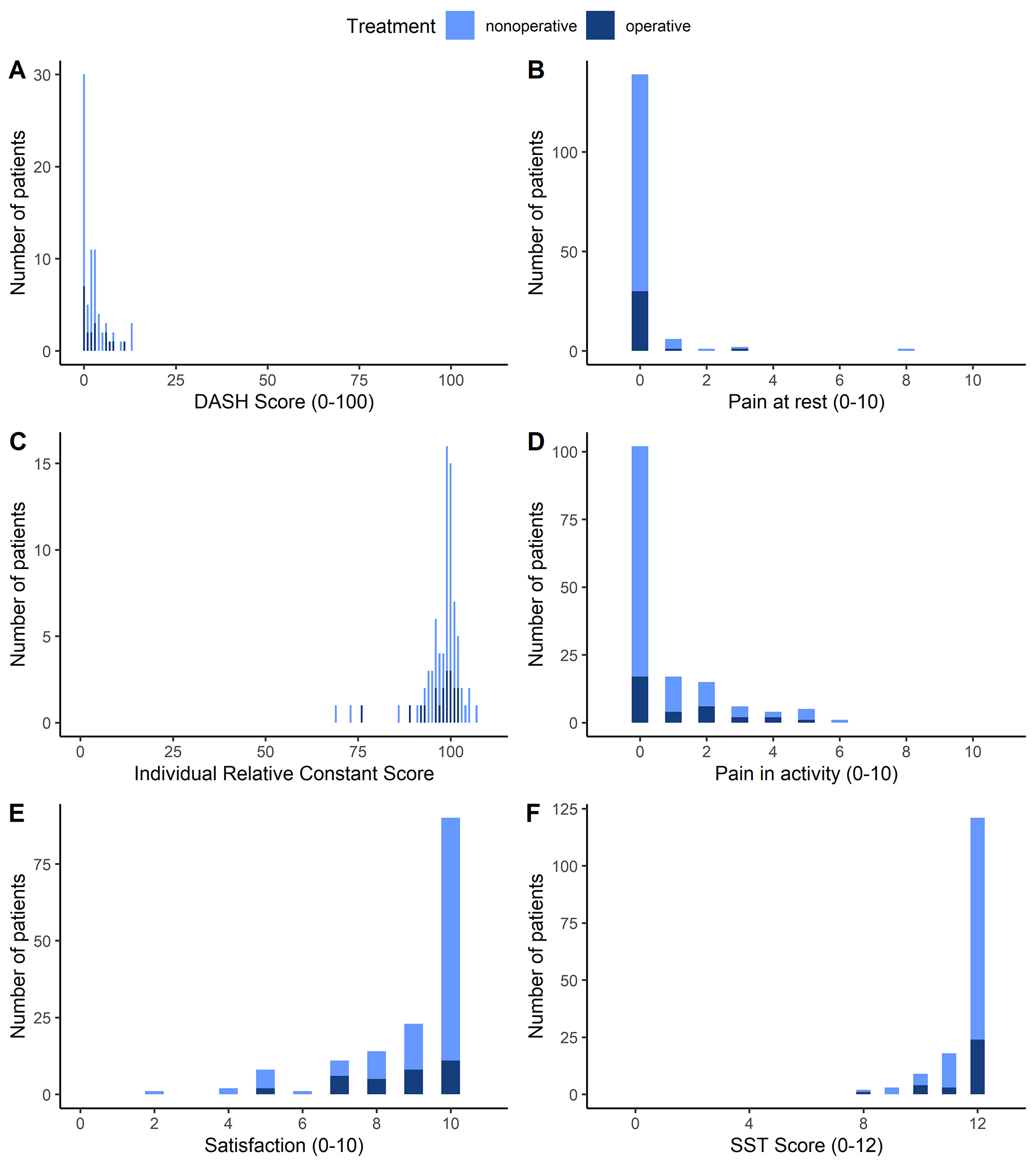
Dr. Marc Swiontkowski, JBJS Editor-in-Chief, discusses a new study assessing the long-term outcomes of proximal humeral fractures sustained in adolescence. Treating fractures involving the physes
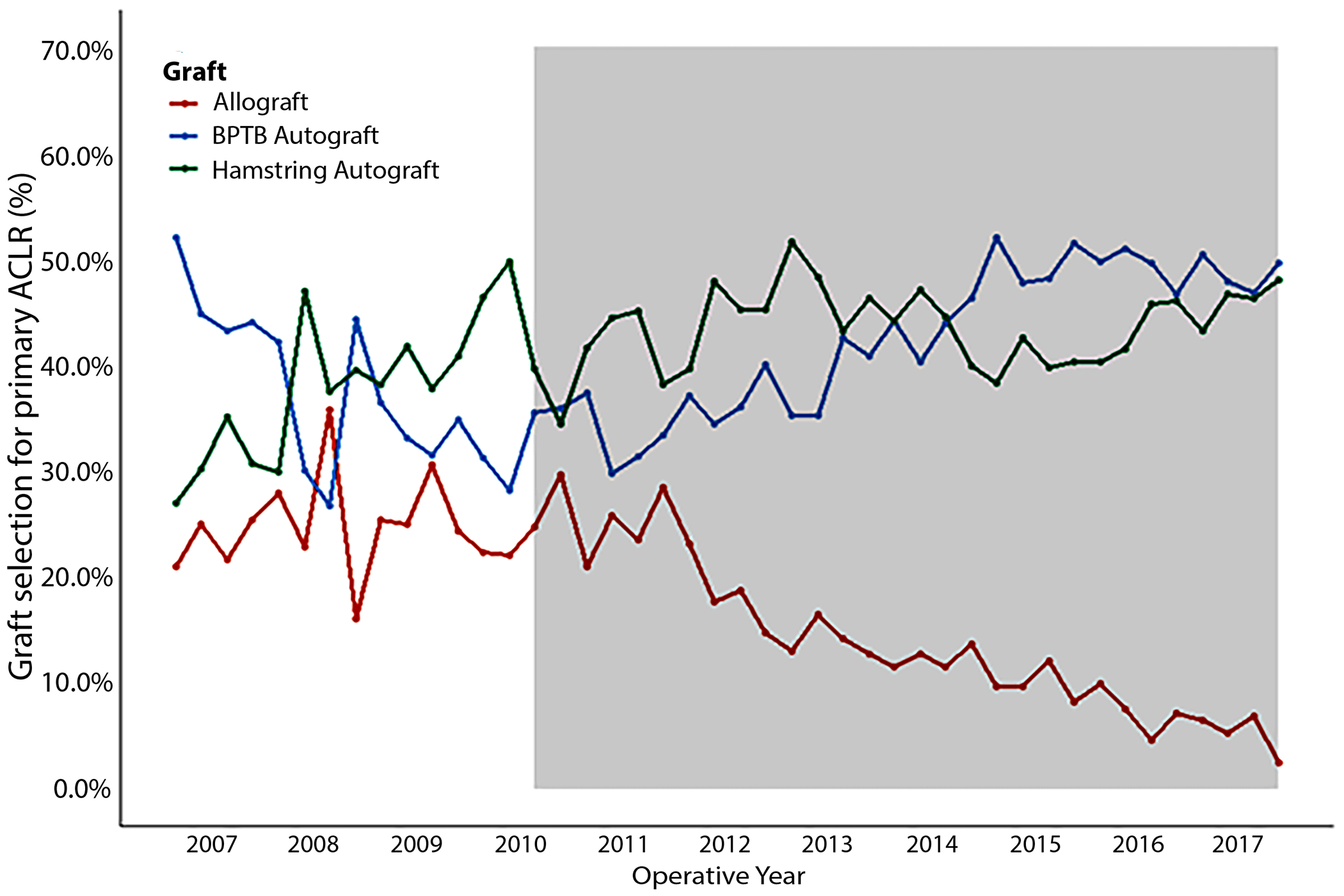
This post comes from Dr. Matt Schmitz, JBJS Deputy Editor for Social Media. He reflects on a new study evaluating the impact of an allograft-reduction
The relationship between surgical site infection and preoperative corticosteroid injection for various procedures, findings on the long-term effectiveness of corticosteroid injection versus carpal tunnel release

